Introduction
Many people have problems with their toe and or fingernails. Often various discoloring and deformities bother patients for aesthetic reasons. But nail changes can also be caused by diseases, which should be further examined and treated by a dermatologist who is experienced with treating nail diseases. Changes in toenails mostly result from foot or nail fungus, but there are other causes that also lead to changes in the nails on both the fingers and toes. They can be serious causes which can be treated by our dermatologists in derma competence center in Zurich Enge.
Table of contents
- Which kinds of nail fungus are there?
- Which nail changes are normal and occur over the course of life?
- Traumatic nail changes caused by injury.
- Birthmarks under the finger- or toenails or in the nail bed.
- Nail changes with eczema or psoriasis.
- What can nail changes caused by inflammatory skin diseases look like?
- Treatment of nail changes in eczema or psoriasis.
- Nail fungus – recognize, diagnose, treat
- What does nail fungus look like?
- How do we get nail fungus?
- How is nail fungus diagnosed?
- How is nail fungus treated?
- Basics: How can you fight nail fungus?
- Treating nail fungus externally:
- Treating nail fungus internally:
- Treating nail fungus with laser
- Nail Fungus and Home Remedies
- Conclusion
1. Which kinds of nail fungus are there?
There are various changes to the fingernails and toenails. Some of these can be triggered by diseases. The most common disease in this case, is probably nail fungus. Changes in the nails, however, can also occur that are not caused by disease or heredity.
These changes, also called nail dystrophies or onychodystrophies, are for example:
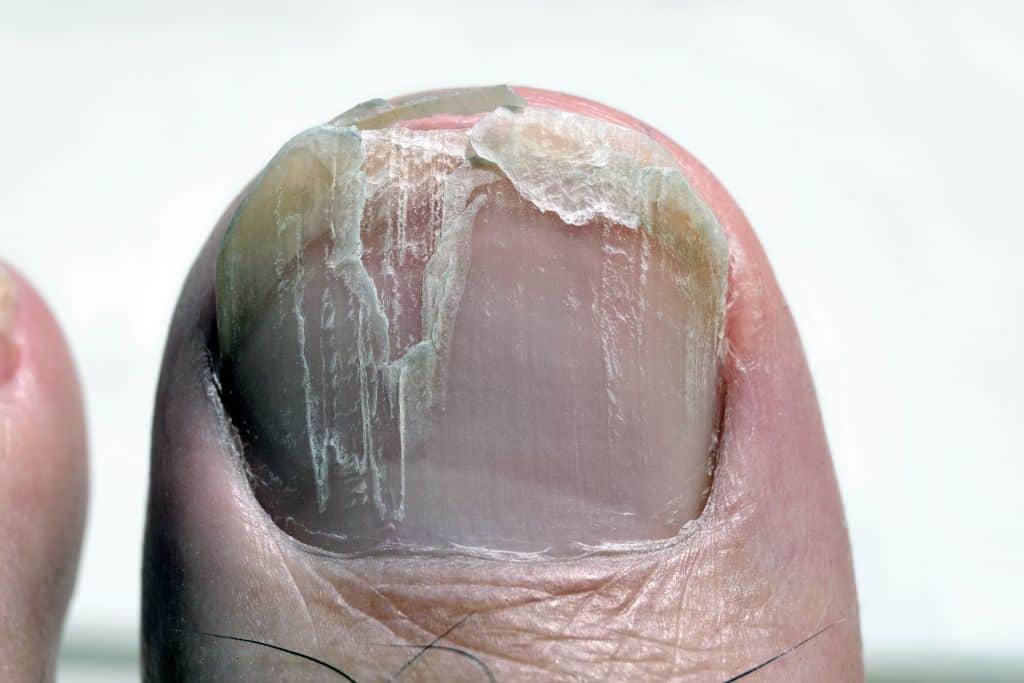
Onychorrhexis
Describes the increased brittleness or splitting of the nail plate. It occurs in the early stages of nail fungus, but also in other diseases or nail symptoms, such as severe vitamin deficiency.
Onychorrhexis, brittleness of the nail can also be a symptom of toenail fungus. ©Sweeann – AdobeStock
Onycholysis
Onycholysis is the detachment of a nail from the nail bed due to various causes, such as severe eczema.
Horizontal ridging
Deep transverse ridges (also called Beau’s lines) indicate that the growth of the nail was disturbed. These often occur after injuries to the nail matrix due to, for example, inflammation or after incorrect manicure/pedicure of the nail bed.
2. Which nail changes are normal and occur over the course of life?
Certain changes in nails over the course of life are normal.
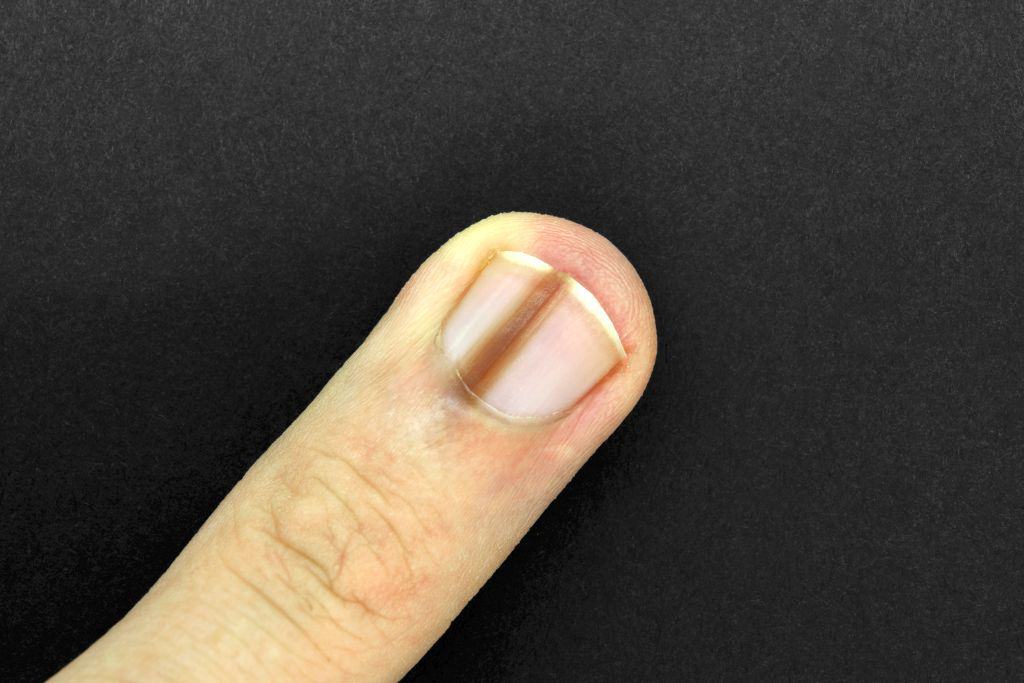
Koilonychia, a spoon-shaped ending, especially of the big toenails, with the formation of a gap under the edge of the nail, is normal in infancy and young children.
These usually grow out by kindergarten age and no not need to be treated. This is often misdiagnosed as toenail fungus.
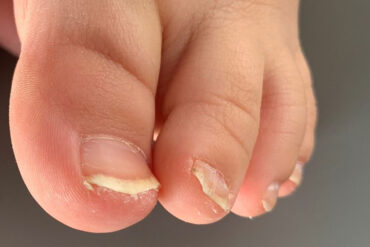
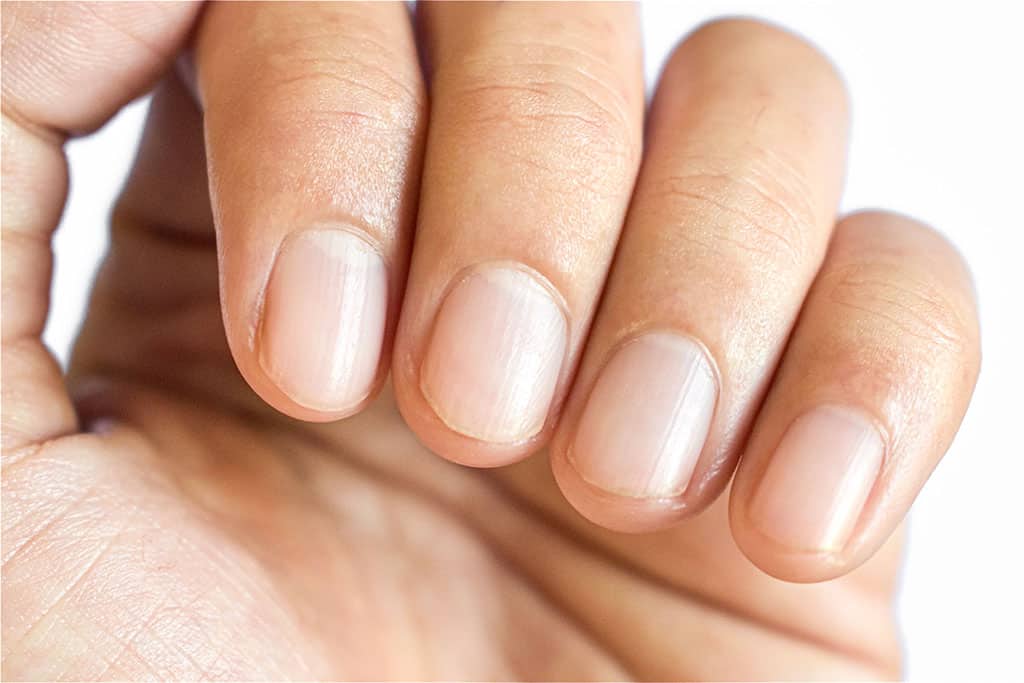
Normal nail changes in infants and young children, rarely nail fungus.

Normal nail changes with mostly not a nail fungus ©ohishiftl – AdobeStock
During the course of adult life, more and more whitish streaks can appear in the nails. Severity varies for each individual.
White spots also appear in some people as they get older.
These discolorations or nail changes are almost never, as wrongly assumed, triggered by deficiencies (vitamin, calcium, etc.).
Only an extreme undersupply of the body with vitamins or internal organ diseases can lead to nail changes. A slight initial stage of nail fungus should however be ruled out. This initial stage of nail fungus can become noticeable through very subtle discoloration.
3. Traumatic nail changes caused by injury.
Traumatic nail changes are almost as common as nail fungus. They are caused by external injuries to the nail and the nail bed and nail-forming apparatus.
It is not uncommon for many patients to show such changes to a dermatologist, like Dr Schnitzler in his dermatology practice in Zurich Enge.
The differentiation from nail fungus or other causes of nail changes should then be ruled out.
3.1. What can traumatic nail changes look like?
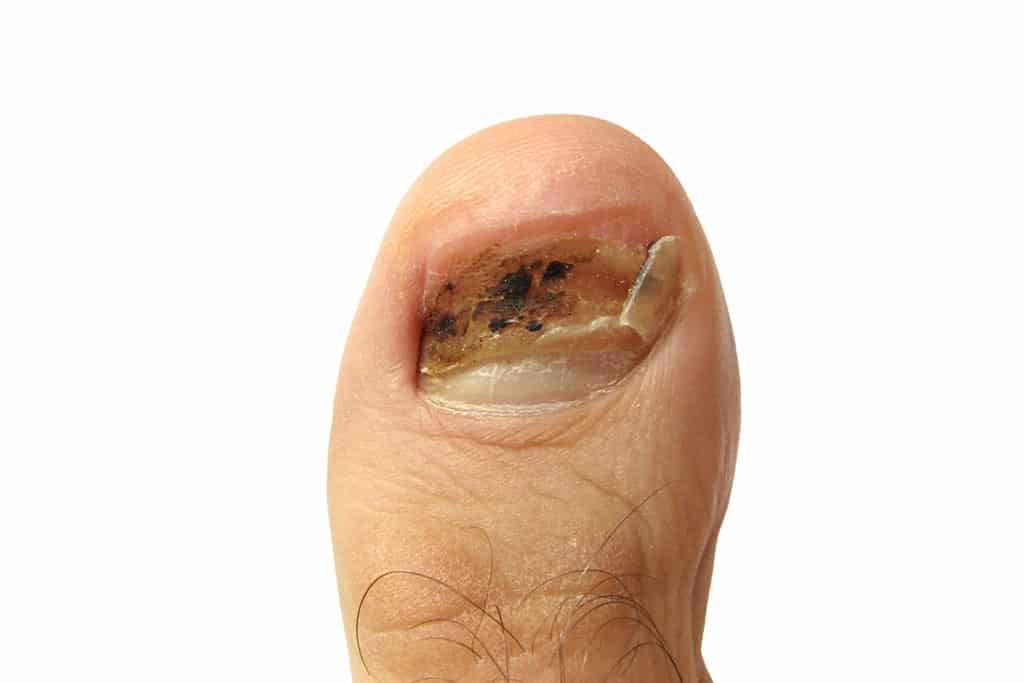
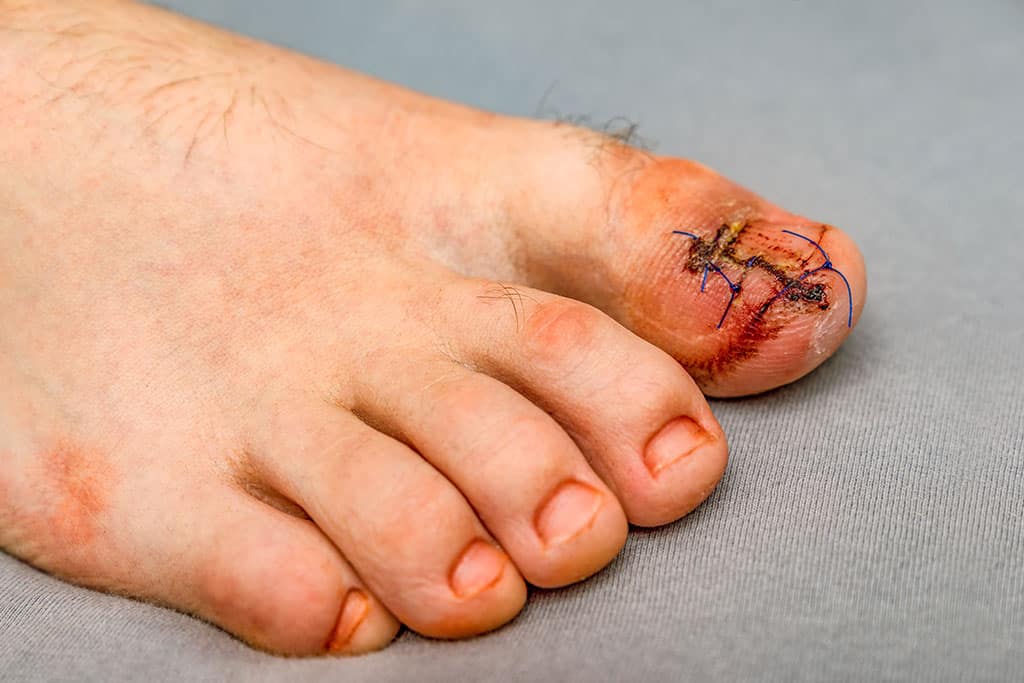
Even the smallest, unnoticed injury usually leads to reddish-brown discoloration of the nail. The discoloration can go as far as complete black-blue-violet discoloration of the entire nail. In some cases, the nail can also lift off and become detached from the nail bed. These changes, especially on the toenails, can be very similar to a brown toenail fungus.
If a scar has formed in the nail bed, this often results in a nail growth disorder with longitudinal cracking and brittleness of the nail at the groove in the nail plate.
3.2. How is nail trauma treated?
Nowadays such traumas are only treated with protective measures. You let the nail come off on its own or the injury grow out.
Occasionally, suitable care ointments and creams with urea, such as supporting nail laquears, lead to an improvement in nail growth and to the closure of the groove in the nail.
Dietary supplements with zinc, biotin and other ingredients that promote nail growth can have a supportive effect.
The operative “pulling” of the nail is nowadays only rarely performed.
If an operation is required, this should be done with the nail preserved as much as possible.
However, a dermatologist should rule out tumors under the nail as the cause of nail changes, and care should be taken to avoid additional infection.
4. Birthmarks under the finger- or toenails or in the nail bed.
Birthmarks can be under the nail, although they are quite rare.
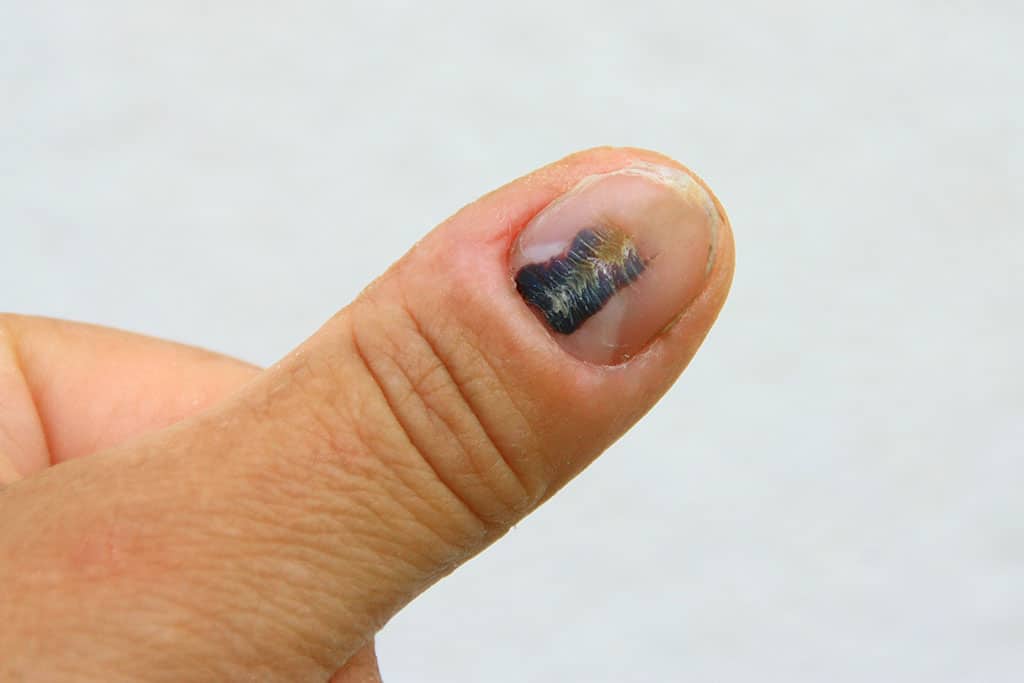
What do birthmarks under nails look like?
Birthmarks under the nails usually appear as homogeneous brown vertical lines that run through the entire nail.
Do birthmarks under the nails need to be treated?
No, but they should be examined by an experienced dermatologist. It must be ruled out that it is not a melanoma in the nail bed. A nail fungus, a rather rare black toenail fungus, should also be ruled out. This can also cause black or brown discoloration of the nail.
5. Nail changes with eczema or psoriasis.
5.1. What can nail changes caused by inflammatory skin diseases look like?
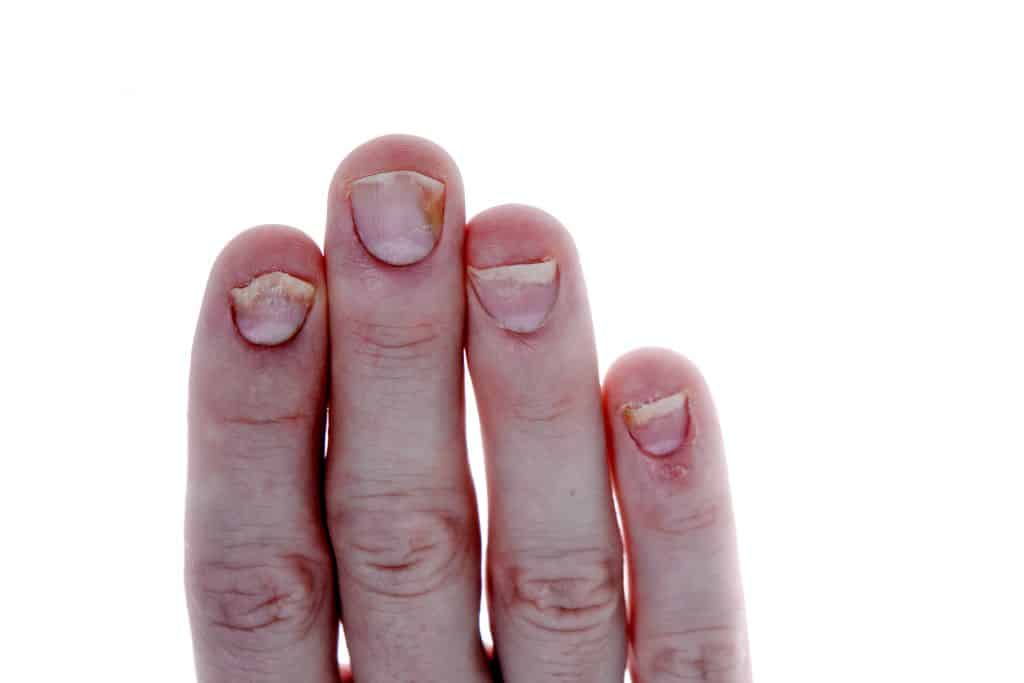
Inflammatory skin changes that spread to the nail bed can lead to nail changes.
These lead to abnormal nail growth, which often manifests itself as waves in the nail plate with transverse grooves.
Yellowish spots can also form in the nail. These so-called oil drops are very common with psoriasis. These oil drops should be shown to an experienced dermatologist. It is important to distinguish them from a fungal infection that looks very similar.
5.2. Treatment of nail changes in eczema or psoriasis.
Treatment is by addressing the underlying skin condition. This is followed by a healing of the nail deformities, albeit delayed.
These inflammatory skin diseases often form the basis for toenail fungus or fingernail fungus due to the weakened immune system of the skin.
6. Nail fungus – recognize, diagnose, treat
Toenail fungus is the most common cause of discoloration and changes in human nails. It is also known as onychomycosis. It is mostly found on the toenails as the widespread toenail fungus. But also, it is not uncommon for fingernails to be infected with nail fungus. Especially in the early stages, nail fungus is difficult to differentiate from other diseases causing nail abnormalities.
6.1. What does nail fungus look like?
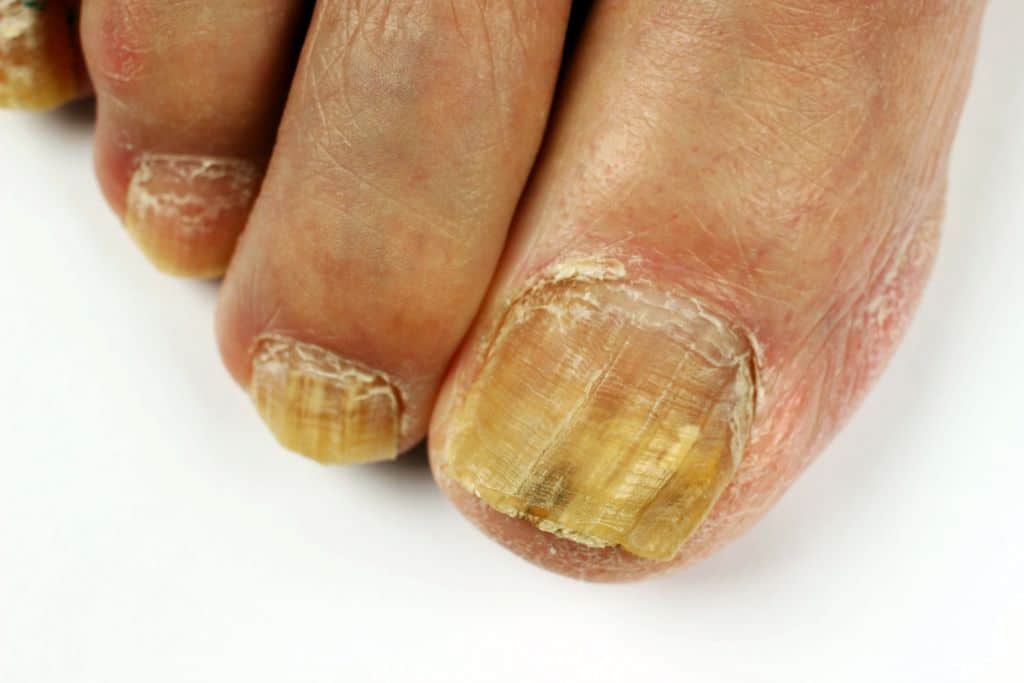
The appearance of a nail affected by onychomycosis can sometimes be very different. In the initial stage of the nail fungus, only slight yellowish whitish discolorations are visible, mostly starting from the edges of the nail.
If the nail fungus is not treated, the discoloration usually spreads and can affect the entire nail. In most cases, the onychomycosis spreads from one nail to the other. Eventually all nails can be affected.
In addition to discoloration, the nail can increase in thickness. Crumbly yellow nail debris is usually found under the solid nail plate.
Then, as the onychomycosis progresses, nail deformities also develop. Some of the nails may become massively grotesquely deformed, especially in the final stage.
In rare cases, pain, reddening of the nail fold and inflammation of the nail bed also occur.
6.2. How do we get nail fungus?
Onychomycosis often develops after a fungus infection that initially only affects the feet. Since this “athlete’s foot” can go unnoticed, the infection can spread to the nail.
Onychomycosis is often caused by filamentous fungi (dermatophytes). Sometimes mold or yeast are also responsible for the infection.
In principle, the fungi can attack all calloused parts of the body (skin, nails, and hair). The fungus mainly feeds off keratin.
Risk factors are, for example, a damp environment in closed shoes (“sweaty feet”), the use of communal showers (sauna, sports club, swimming pool), frequently damp/wet hands, metabolic and immune diseases (e.g., diabetes mellitus or an immune deficiency), circulatory disorders, smoking, possibly also vitamin and zinc deficiency. Toenail fungus is more common with age.
6.3. How is nail fungus diagnosed?
Nail fungus can usually be quickly diagnosed by an experienced dermatologist, as with the dermatologists at derma competence center in Zurich Enge.
An additional removal of nail material and the subsequent microscopic examination can provide certainty.
Cultivation (culture) in the practice laboratory underpins the diagnosis and provides information about which type of fungus is the cause of the nail fungus disease.
6.4. How is nail fungus treated?
6.4.1. Basics: How can you fight nail fungus?
Proper hygiene is the key to successfully fight nail fungus.
Stockings and socks should be washed with a suitable supplemental detergent and, whenever possible, on high temperatures.
In addition, all shoes that are worn should be treated with special antifungal agents (e.g., a spray or powder). This can prevent reinfection.
6.4.2. Treating nail fungus externally:
In addition to care measures to strengthen the skin and nails, antifungal nail lacquers are very effective. They penetrate the nail and fight against the fungus.
In this case, the nail should be filed beforehand and prepared with disinfection.
There are preparations that should be applied daily (Ciclopoli) or weekly (Amorolfine). The active ingredients in Ciclopoli and Amorolfine penetrate the nail and fight nail fungus. Certain nail creams also help to treat nail fungus.
6.4.3. Treating nail fungus internally:
If topical therapy with Ciclopoli or Amorolfine is unsuccessful, or if more than 40% of all nails or 40% of a nail are affected, systemic therapy, i.e., therapy with prescription antifungal pills, should be carried out. These pills (there are various very effective preparations, e.g., Terbinafine) despite widespread opinion, are quite free of side effects.
There are also additional application schemes, such as shock therapy in contrast to continuous tablet intake. Accompanying blood tests can sometimes be helpful in identifying side effects as early as possible
6.4.4. Treating nail fungus with laser

The additional laser therapy for nail fungus usually leads to a faster healing and promotes new growth of a healthy nail. Laser therapy is well suited additional therapy to combat nail fungus.
With laser therapy, the affected nail is treated with a nail fungus laser that is specially designed for this purpose. This treatment leads to an almost imperceptible heating of the nail. Only the fungus is damaged.
There are almost never any side effects with nail fungus laser treatment.
The success of the modern way of treating nail fungus speaks for itself. Unfortunately, it is often not covered by health insurance. However, this can be coordinated with the patient’s health insurance company in advance of the nail fungus laser treatment.
6.4.5. Nail Fungus and Home Remedies
Home remedies can only help to a limited extent with nail fungus!
There are a variety of home remedies for nail fungus. They can mostly be found in naturopathic literature and on the Internet.
These are extremely versatile and range form baths in vinegar or vinegar-water to urine therapies (own urine). Treatment of nail fungus that is completely free of side effects is often promised.
In reality, the truth is all too often much different. Although these home remedies can occasionally achieve an improvement of the nail fungus.
Unfortunately, the sometimes-long-term use of home remedies against nail fungus usually only delays the precise diagnosis and worsens the situation.
The advanced nail fungus is then more difficult to treat.
7. Conclusion
Discoloration and deformation of nails on fingers and toes is common. They are in most cases triggered by fungal infections or injuries. The cause should always be examined. If you suspect nail fungus, be it toenail fungus or fingernail fungus, you should see an experienced dermatologist. They can determine the type of fungus. Nail fungus, especially in its early stages, is easy to treat.

Autor - Dr. med. Hero P. D. Schnitzler
I am Dr. Hero P. D. Schnitzler and founded the derma competence center in Zurich Enge in 2015, which I have been managing with heart, soul and professional competence ever since.
I am a member of various Swiss and international professional societies and a long-time lecturer for aesthetic laser medicine (D.A.L.M.) at the University of Greifswald, and for the Swiss skills program FMCH laser treatments of the skin.